Best Fungal Acne Skincare Routine

I completely understand the frustration of dealing with those pesky, itchy bumps that just won’t go away, no matter what you do.
If you’ve tried traditional acne products and they haven’t cleared your bumps, it is possible you may have fungal acne. This is not your average acne and requires a different, more specific approach.
I’ll be giving you the step-by-step process to formulate a fungal acne routine that works!
The guide has everything: safe products to use, the ingredients to avoid, morning and night routines, and of course, cost-effective options.
I’ve collated research-based dermatologists recommendations and tested options for clearing these breakouts.
You’ll learn how to identify fungal acne, what are the causes, and how to achieve a clear complexion.
Let’s do this together.
Why Your Current Routine Isn’t Working
Most people treat fungal acne like regular acne, which only makes the problem worse and prolongs breakouts.
You’ve probably been using benzoyl peroxide, retinoids, or antibiotics. These work for bacterial acne but do nothing for yeast overgrowth.
Fungal acne needs antifungal treatments, not antibacterial ones. That’s why your usual products keep failing.
Worse, some skincare ingredients actually feed the yeast. That face oil or rich moisturizer? They’re making it thrive.
Switch to fungal-safe products and you’ll see results within weeks, not months.
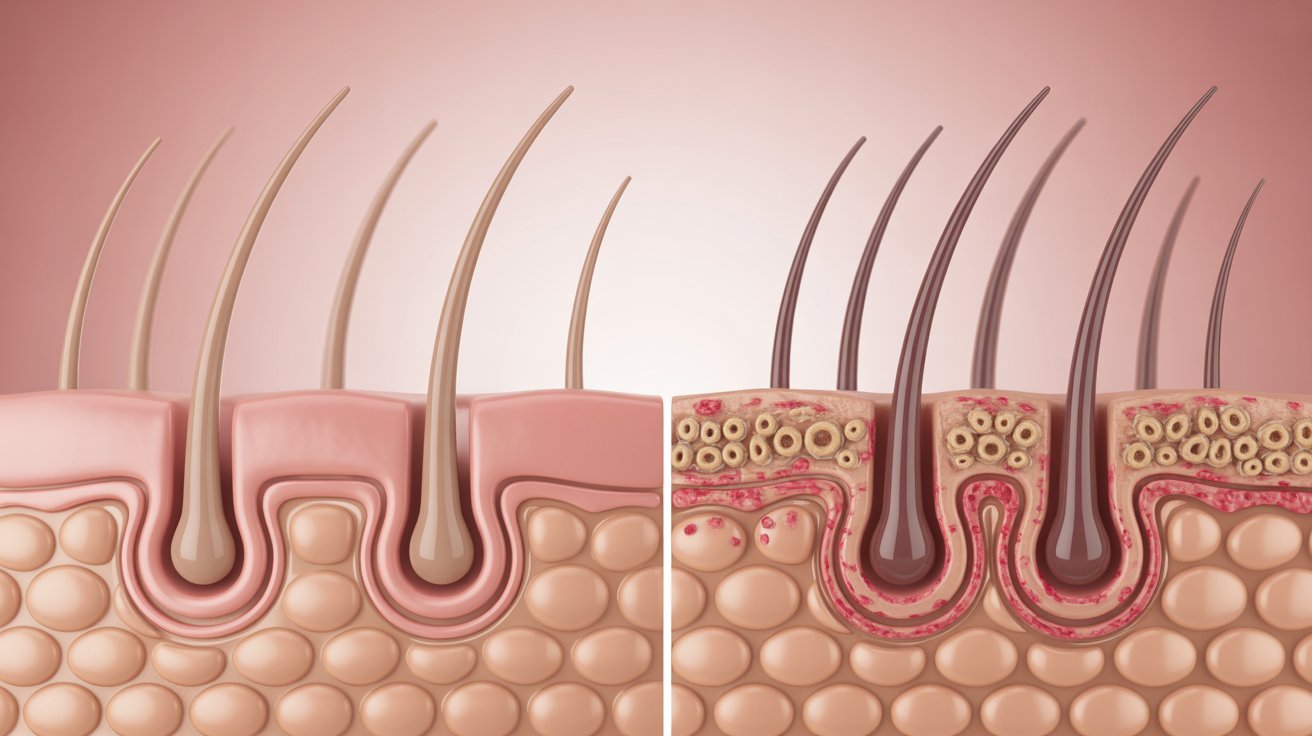
Understanding Fungal Acne
Fungal acne looks like regular acne, but it requires a completely different treatment approach to clear your skin.
What Is Fungal Acne?
Fungal acne isn’t really acne at all. It’s called Malassezia folliculitis.
A yeast called Malassezia lives naturally on your skin. When conditions get too warm and moist, this yeast multiplies too fast. It gets trapped inside your hair follicles and causes inflammation.
Regular acne comes from bacteria and clogged pores. Fungal acne comes from yeast overgrowth. That’s why regular acne treatments don’t work on it. Some can even make it worse.
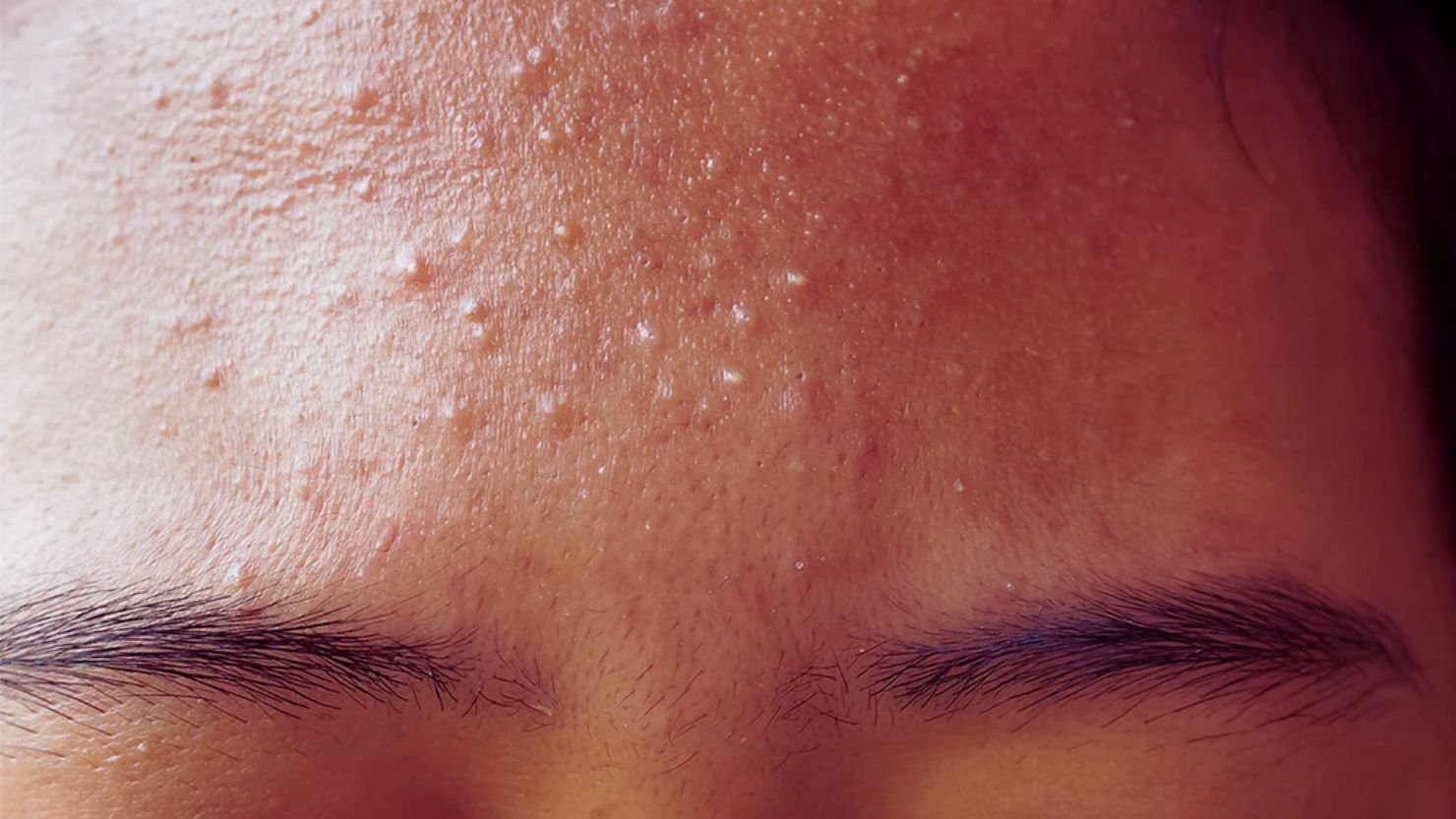
How to Identify Fungal Acne
Fungal acne has specific signs that set it apart.
The bumps are small, uniform, and clustered together. They’re usually red or skin-colored and all look roughly the same size.
The biggest difference? Fungal acne itches. Regular acne rarely itches, but fungal acne can be seriously itchy.
You’ll typically see it on your forehead, temples, hairline, chest, upper back, and shoulders. These are areas where you sweat more and produce more oil.
The bumps don’t have a “head” or whitehead like bacterial acne. They feel like tiny, raised bumps under the surface.
Causes and Triggers
Several factors contribute to fungal acne development, from environmental conditions to your daily habits and diet choices.
Main Causes
- Excess oil and sweat: create the perfect environment for yeast to grow. When your skin produces too much sebum, it feeds the Malassezia yeast.
- Hot and humid weather: makes everything worse. Heat and moisture let yeast multiply faster. That’s why fungal acne often flares up in summer.
- Tight workout clothes: trap sweat against your skin. The yeast loves this warm, damp environment. Staying in sweaty clothes too long is asking for trouble.
- Taking antibiotics: for bacterial acne can backfire. Antibiotics kill good bacteria on your skin, letting yeast take over and grow out of control.
- Heavy, occlusive skincare products: block your pores. They trap oil and sweat underneath, giving yeast exactly what it needs to thrive.
Lifestyle and Diet Factors
- High-sugar and refined-carb diets: can feed yeast from the inside out. The yeast consumes these sugars and grows faster.
- Skipping showers after workouts: is a major trigger. Sweat sitting on your skin for hours creates ideal conditions for fungal growth.
- Stress weakens your immune system: When your body can’t regulate yeast levels properly, breakouts happen more easily.
Dermatologist-Approved Fungal Acne Skincare Routine
A strategic daily routine with antifungal products and safe ingredients helps control yeast overgrowth and restore clear skin.
Morning Routine (AM)
Start with a gentle, oil-free cleanser that contains antifungal ingredients. Look for zinc pyrithione or ketoconazole-based formulas. These ingredients actively fight the yeast while cleaning your skin.
Apply a lightweight treatment next. Niacinamide serums work great because they calm inflammation without feeding the yeast. Keep the formula simple and water-based.
Follow with a fungal acne-safe moisturizer. It should be non-comedogenic and completely oil-free. Your skin still needs hydration, even with fungal acne.
Finish with broad-spectrum SPF protection. Choose an oil-free, fragrance-free sunscreen. Mineral sunscreens with zinc oxide are usually safe options.
Evening Routine (PM)
Start with a double cleanse if you wore makeup or sunscreen during the day. Use a fungal-safe micellar water first. Then wash with your antifungal cleanser.
Apply your targeted antifungal treatment. Ketoconazole cream, clotrimazole, or sulfur-based products work well. These are your main weapons against the yeast.
Finish with a soothing, oil-free moisturizer. This helps repair your skin barrier while keeping the yeast under control. A healthy barrier prevents future flare-ups.
Weekly Treatments and Maintenance
Regular exfoliation and specialized treatments help prevent fungal acne buildup while maintaining clear, healthy skin between daily routines.
Exfoliation (1-2x Weekly)
Chemical exfoliants are your best friend. Salicylic acid and azelaic acid both work well for fungal acne. They remove dead skin cells without creating micro-tears.
Salicylic acid gets into your pores and clears out buildup. Azelaic acid fights both yeast and inflammation.
Skip the physical scrubs entirely. Rough scrubbing can damage your skin barrier. Oil-heavy exfoliants feed the yeast and make things worse.
Antifungal Masks and Treatments
Sulfur masks are incredibly effective. Sulfur has natural antifungal and antibacterial properties. Use these masks once or twice a week for maintenance.
Ketoconazole masks provide stronger antifungal action. They’re great for active breakouts or stubborn areas.
Tea tree oil can help mild cases when properly diluted. Mix a few drops with a carrier that’s fungal-safe. Never apply it directly to your skin undiluted.
Best Fungal Acne-Safe Products (Dermatologist & Budget Picks)
These dermatologist-recommended and budget-friendly products contain safe ingredients that won’t feed Malassezia yeast while treating your skin.
Cleansers:
iUNIK Centella Bubble Cleansing Foam is gentle and fungal-safe. It cleans without stripping your skin. The centella soothes inflammation.
Nizoral Anti-Dandruff Shampoo works as an antifungal wash for your face and body. It contains ketoconazole, which directly fights yeast. Leave it on for a few minutes before rinsing.
Treatments:
Pyunkang Yul Acne Spot Cream: targets problem areas without harsh ingredients. It’s simple and effective.
Clotrimazole or Ketoconazole Creams: are available over-the-counter or by prescription. These are proven antifungal medications that work fast.
Moisturizers:
The beauty of Joseon Dynasty Cream: is completely oil-free. It hydrates without feeding yeast. The formula is clean and minimal.
COSRX Oil-Free Ultra-Moisturizing Lotion: keeps skin balanced. It’s lightweight and absorbs quickly.
Sunscreens:
Purito Daily Go-To Sunscreen: protects without clogging pores. It’s fungal-safe and comfortable for daily wear.
The beauty of Joseon Relief Sun: offers broad protection. The formula is gentle and won’t trigger breakouts.
Pro Tip: Always patch-test new products on a small area first. Avoid ingredients that feed Malassezia, including olive oil, esters, and polysorbates.
Fungal Acne-Safe Ingredients to Look For
Knowing which ingredients help and which ones harm your skin makes choosing safe products much easier and faster.
Safe Ingredients
Niacinamide: calms inflammation and strengthens your skin barrier. It controls oil without feeding yeast.
Hyaluronic acid: provides hydration without any risk. It’s a water-binding ingredient that keeps skin plump.
Glycerin: attracts moisture to your skin without feeding fungal growth.
Squalane: (not squalene) is safe to use. Make sure the label says squalane with an “a.”
Aloe vera: soothes irritated skin. It’s anti-inflammatory and completely safe.
Ingredients to Avoid
Coconut oil, olive oil, and most natural oils: feed the yeast. They’re Malassezia’s favorite food.
Esters: like isopropyl myristate and isopropyl palmitate trigger fungal acne. Check ingredient lists carefully.
Polysorbates and fermented ingredients: can encourage yeast growth. Avoid these in your products.
Dermatologist Advice for Long-Term Management
Consistent habits and preventive measures keep fungal acne under control and reduce the chance of future flare-ups.
Maintain antifungal hygiene as part of your routine. Use antifungal washes regularly, even after your skin clears. This prevents the yeast from building up again.
Wear loose, breathable fabrics whenever possible. Cotton and moisture-wicking materials are best. They let your skin breathe and reduce sweat buildup.
Shower immediately after workouts. Don’t let sweat sit on your skin. Change out of damp clothes right away.
See a dermatologist for persistent cases. If topical treatments aren’t working after a few weeks, you might need oral antifungal medication. Prescription options work faster and more completely.
Budget-Friendly Tips
You don’t need expensive products to treat fungal acne effectively, smart shopping and multipurpose items save money while clearing skin.
- Use multipurpose antifungal products to save money: Nizoral shampoo works as a face wash, body wash, and scalp treatment. One bottle covers multiple needs.
- Focus on the essentials first: a good cleanser, one effective treatment, a basic moisturizer, and sunscreen. You don’t need ten products.
- K-beauty brands offer great value: They often have simple, clean ingredient lists. Many are naturally fungal-safe and cost less than Western brands.
Conclusion
I experienced fungal acne as well, I also wasted months using the wrong products before I finally figured it out.
When I finally switched to a proper fungal acne skincare routine, my skin had completely cleared in only three weeks.
Stay consistent with the methodology we covered in this guide. It takes time for your skin to heal, but it will.
If you don’t see any substantial improvements after a few weeks, it’s a good idea to get some extra help from your dermatologist.
Leave a comment and share your results! Your experience might help someone else get clear skin!
Frequently Asked Questions
How long does it take to clear fungal acne?
Most people see improvement within 2-4 weeks of using the right antifungal products. Severe cases may take 6-8 weeks. Consistency matters more than speed.
Can I use regular acne products on fungal acne?
No, regular acne products won’t work and might make things worse. Fungal acne needs antifungal treatments like ketoconazole or sulfur, not benzoyl peroxide or salicylic acid alone.
Is fungal acne contagious?
No, fungal acne isn’t contagious between people. The Malassezia yeast already lives on everyone’s skin. It only causes problems when it overgrows due to specific conditions.
Can diet affect fungal acne?
Yes, high-sugar and high-carb diets can feed yeast from the inside. Reducing sugar intake may help control fungal acne, though topical treatments are still essential.
Should I stop moisturizing if I have fungal acne?
Never skip moisturizer. Your skin still needs hydration. Just choose oil-free, fungal-safe moisturizers. A damaged skin barrier makes fungal acne harder to treat.