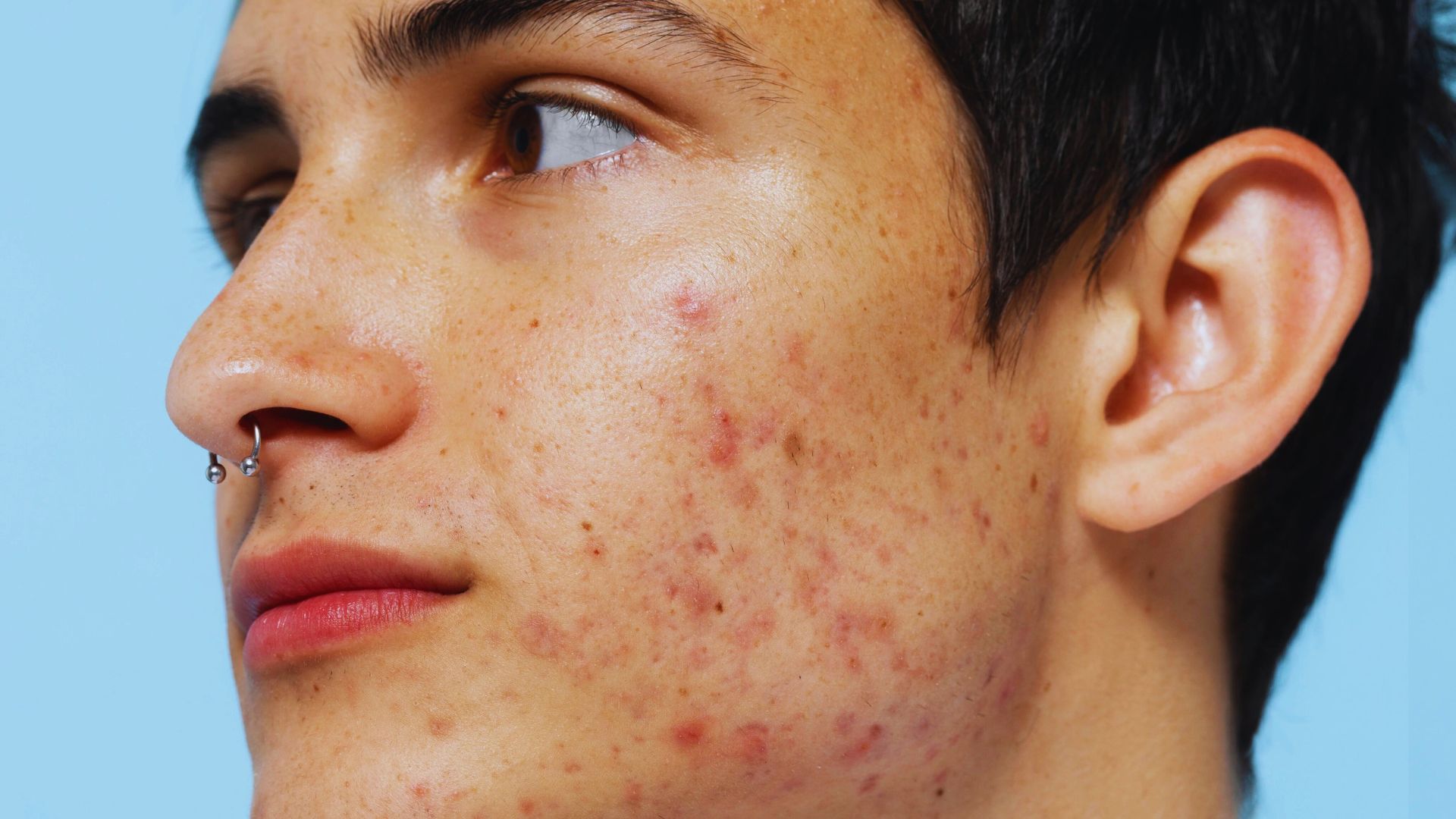
Fungal Acne vs Bacterial Acne Explained

Dealing with breakouts can be frustrating, especially when you can’t figure out what’s causing them. Fungal acne vs bacterial acne often gets mixed up because they look alike.
But here’s the truth: they come from different sources and need different fixes. I’ve spent years helping people identify their skin issues, and getting the right diagnosis changes everything.
In this article, I’ll show you how to tell them apart, what triggers each type, and which treatments actually work.
You’ll learn the key differences, spot the symptoms, and finally get clear on what your skin needs.
Understanding Acne Types and Why Diagnosis Matters
Most people assume all bumps are regular acne. That’s not always true. Sometimes what looks like acne is actually a yeast problem. Your skin hosts different organisms, and when yeast multiplies, it creates bumps that mimic traditional pimples.
Here’s the problem: using the wrong treatment makes things worse. I’ve seen people use acne medication for months with zero results.
They’re treating bacterial acne when they actually have fungal acne. The opposite happens too. Wrong treatments make your skin angrier. Getting the right diagnosis saves you time and frustration.
A dermatologist can test your skin and confirm what you’re dealing with. This leads to faster, better results.
Here’s your revised section with a one-line description after the intro and a clean difference table format for better SEO and featured snippet potential.
Fungal Acne vs Bacterial Acne What’s the Difference?
These two conditions look similar but have completely different causes, requiring opposite treatment approaches for clear skin.
What Is Fungal Acne?
Fungal acne comes from Malassezia yeast that naturally lives on your skin. When heat, sweat, or humidity create the right conditions, this yeast multiplies and triggers inflammation in your hair follicles.
You’ll notice small, uniform bumps that appear in clusters and often feel itchy. These breakouts commonly show up on your forehead, chest, back, and shoulders. They get worse when you sweat or during humid weather.
What Is Bacterial Acne?
Bacterial acne happens when Cutibacterium acnes bacteria multiply inside pores clogged with oil and dead skin. This creates whiteheads, blackheads, pustules, and cysts that vary in size.
The breakouts can be painful or inflamed, especially deeper cysts. This type is often linked to hormones and excess oil production. Unlike fungal acne, the bumps don’t look uniform and appear in different shapes and sizes.
Fungal Acne vs Bacterial Acne Key Differences
These two conditions look similar but have completely different causes, requiring opposite treatment approaches for clear skin.
| Feature | Fungal Acne | Bacterial Acne |
|---|---|---|
| Cause | Overgrowth of Malassezia yeast | Overgrowth of Cutibacterium acnes bacteria |
| Appearance | Small, uniform bumps | Mixed sizes and lesion types |
| Itching | Common symptom | Rare |
| Common Locations | Forehead, chest, back, shoulders | Face, jawline, back, chest |
| Main Triggers | Sweat, humidity, tight clothing | Hormones, excess oil, pore-clogging products |
| Treatment Approach | Antifungal products | Antibacterial treatments |
Symptoms and Appearance How to Tell Them Apart
Learning to recognize specific visual and physical clues helps you identify which type of acne you have.
Signs of Fungal Acne
The bumps are small and identical. Line them up and they look like twins. This uniformity is a major clue. Itching is common and persistent, which regular pimples don’t usually cause.
Check where the bumps appear-they love your forehead, chest, and back, especially areas that trap sweat. Run your hand over the area and you’ll feel lots of tiny, raised bumps clustered together.
Signs of Bacterial Acne
Bacterial acne shows mixed lesion sizes. You’ll have small whiteheads next to large cysts. Nothing matches. Pus-filled pimples are common with white or yellow tips.
The breakouts feel painful or inflamed, especially deep cystic acne that creates tender spots under your skin. You’ll often see redness around each pimple. The area looks angry and swollen.
Fungal Acne & Bacterial Acne on Forehead and Back
Both types show up on the forehead and back, but patterns differ. Fungal acne on the forehead creates a field of uniform bumps across your hairline and temples. Sweat from workouts or wearing hats triggers flares. On the back, it follows sweat patterns where moisture collects, like along the spine or shoulder blades.
Bacterial acne creates random, scattered breakouts that don’t follow moisture patterns. Body acne from bacteria often comes from friction-backpacks, tight shirts, and sports equipment that create pressure points that develop painful bumps.
Causes and Triggers Behind Each Type
Understanding what triggers your breakouts helps you prevent future flares and maintain clearer skin long-term.
Fungal Acne Triggers
Heat and humidity create the perfect breeding ground for Malassezia yeast. Summer months often bring flares. Excess sweating feeds the yeast, so working out can trigger breakouts if you don’t shower immediately afterward.
Tight clothing traps moisture against your skin-synthetic fabrics, sports bras, compression gear, and tight workout clothes all cause problems.
Antibiotic use disrupts your skin’s balance. Antibiotics kill bacteria but not yeast, so when bacteria decrease, yeast can take over. Long-term antibiotic treatment for bacterial acne sometimes causes fungal acne instead.
Bacterial Acne Triggers
Hormonal changes are huge triggers. Periods, pregnancy, and puberty all affect oil production, and more oil means more food for bacteria. Excess oil production clogs pores, making oily skin types struggle more. The sebum creates a perfect environment for bacterial growth.
Comedogenic skincare blocks pores-heavy creams, certain oils, and thick makeup trap debris. Always check if products are labeled non-comedogenic. Genetics play a role too. If your parents had acne, you’re more likely to get it. Your skin type and oil production are partly inherited.
Treatment Options for Fungal Acne & Bacterial Acne
Choosing the right treatment based on your acne type makes all the difference in achieving clear skin.
Fungal Acne Treatment
Antifungal shampoos work wonders for fungal acne. Products with ketoconazole kill Malassezia yeast-use them as a face or body wash and leave on for a few minutes before rinsing.
Selenium sulfide is another option found in dandruff shampoos that targets yeast growth.
Switch to oil-free skincare because Malassezia feeds on certain oils like coconut oil, olive oil, and fatty acids.
Stop using heavy moisturizers and choose lightweight, water-based products instead. For severe cases, a dermatologist might prescribe oral antifungal medication.
Bacterial Acne Treatment
Benzoyl peroxide kills bacteria and comes in different strengths. Start with 2.5% and increase if needed-it also reduces inflammation. Salicylic acid unclogs pores by dissolving the oil and dead skin blocking them.
Use it in cleansers or spot treatments. Retinoids speed up cell turnover and prevent dead skin from clogging pores.
Prescription retinoids work faster than over-the-counter versions. Prescription antibiotics might be necessary-oral antibiotics reduce bacteria from the inside while topical antibiotics work on the surface.
Don’t use antibiotics long-term without monitoring. Birth control pills help hormonal acne in women by regulating hormones that trigger oil production.
Tips to Prevent Fungal and Bacterial Acne
Simple daily habits and lifestyle changes can prevent both types of acne from returning after treatment.
- Use non-comedogenic products only. Check all your makeup, moisturizer, and sunscreen labels.
- Cleanse immediately after sweating. Shower right after workouts or use cleansing wipes if you can’t.
- Avoid heavy oils on breakout-prone areas. Stick to lightweight, oil-free formulas instead.
- Wear breathable fabrics. Choose cotton and moisture-wicking materials over synthetic clothes that trap sweat.
- Change pillowcases every few days. They collect oil, bacteria, and yeast that cause breakouts.
- Keep a consistent skincare routine. Your skin needs regular care without constant product changes.
- Manage stress and stay hydrated. High stress triggers oil production, and water keeps skin healthy.
Conclusion
Fungal acne vs bacterial acne might look the same at first glance, but they need totally different care. I used to throw every product at my breakouts until I learned this lesson the hard way. Once I figured out what I was actually dealing with, my skin improved fast.
Now you have the tools to identify your acne type and treat it right. Stop guessing and start seeing results.
Check your symptoms, match them to what you learned here, and pick the treatment that fits. Got questions or want to share your experience? Drop a comment below.
Frequently Asked Questions
Can you have fungal acne and bacterial acne at the same time?
Yes, you can have both types at once. Treat each type with its specific products for best results.
How long does fungal acne take to clear?
Fungal acne usually clears within 2-4 weeks with proper antifungal treatment. If not, you need stronger medication.
Does fungal acne spread easily?
It doesn’t spread person to person. It can spread on your own body, but it’s about controlling yeast overgrowth.
Why does my acne get worse with traditional acne products?
You likely have fungal acne. Antibiotics and heavy moisturizers feed the yeast. Switch to antifungal products instead.
Should I see a dermatologist for fungal acne?
See a dermatologist if treatments don’t work after 4 weeks or if you’re unsure which type you have.